What is Humeral Interlocking Nail and How is it Used?
The Humeral Interlocking Nail is a vital orthopedic tool. Surgeons use it to treat fractures in the upper arm. This innovative device provides stabilization for the humerus bone. It consists of a solid nail that is inserted into the shaft of the bone. The design allows for screws to lock both ends, ensuring proper alignment.
The procedure involves precise placement and careful consideration. Surgeons must assess the fracture type and angulation. Each case demands tailored planning to achieve optimal results. Patients often experience varying levels of discomfort during recovery. Rehabilitation and physical therapy follow the surgical procedure. Healing time can differ significantly among individuals.
Despite its effectiveness, challenges can arise. Some patients may develop complications. These may include infection or improper positioning of the nail. Continuous monitoring is essential for all postoperative patients. The use of the Humeral Interlocking Nail exemplifies modern surgical advancements. Yet, it highlights the necessity for ongoing research and development.
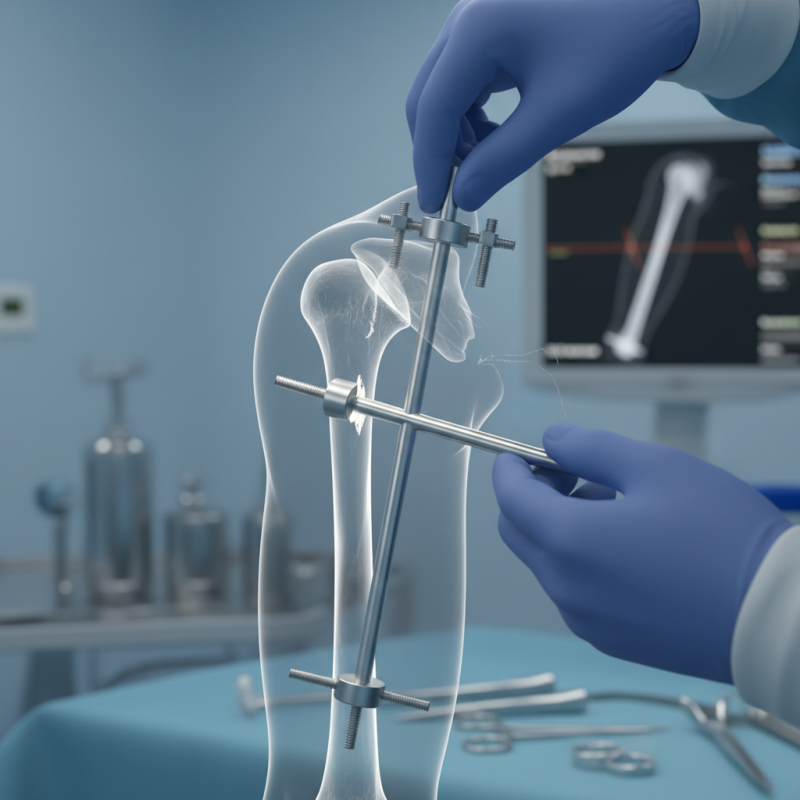
Definition and Overview of Humeral Interlocking Nail
Humeral interlocking nails are specialized surgical implants used in the treatment of humeral fractures. These nails provide stability by engaging both the cortical and cancellous bone. According to the Journal of Orthopaedic Trauma, the use of intramedullary nails for humeral fractures has increased by approximately 30% over the last decade.
The design of these nails allows for minimal soft tissue disruption during insertion. Surgeons can align the fractured bone fragments effectively. However, the procedure still carries risks. Complications like infection or nonunion can occur. In a significant number of cases, around 15%, patients may experience dissatisfaction with their functional outcomes.
Data from recent studies indicate an overall healing rate of 90% in patients using interlocking nails. Despite this, not every case is successful. Surgeons often face challenges with proper nail sizing and placement. Each unique fracture pattern demands tailored approaches. This adds a layer of complexity to an already intricate procedure. Understanding the nuances of humeral interlocking nails is essential for achieving optimal results.
Indications for the Use of Humeral Interlocking Nail
Humeral interlocking nails are vital in orthopedic procedures. They provide stability for fractures around the humerus. The use of these nails is indicated in complex fractures. Specifically, these include diaphyseal fractures, multiple fractures, or cases where bone quality is compromised.
When an individual has a high-energy injury, surgical intervention may be necessary. The interlocking nail offers a minimally invasive solution. It allows for quicker recovery and less pain. Patients with compromised bone healing may particularly benefit from this technique.
Tips for considering this treatment:
- Discuss all options with your surgeon.
- Understanding the risks is crucial.
- Ensure that your medical history is thoroughly reviewed.
- If you're concerned about recovery time, share those thoughts openly.
Surgical Procedure for Inserting Humeral Interlocking Nail
The humeral interlocking nail is a specialized device used in orthopedic surgery. Its primary purpose is to stabilize fractures in the humerus, particularly in cases that are complex or involve intra-articular injuries. The surgical procedure for inserting this device is quite intricate, requiring a clear understanding of anatomy and precision.
During the surgery, the patient is typically placed under general anesthesia. The surgeon makes an incision near the fracture site on the upper arm. After locating the fracture and ensuring proper alignment, the nail is inserted into the medullary canal of the humerus. Drilling holes for screws follows, which help secure the nail in place. Each step demands careful attention to avoid damaging surrounding tissues or nerves.
While this procedure often leads to successful outcomes, challenges can arise. Surgeons might encounter difficulties in aligning the nail properly or managing any existing complications. Post-operative care is equally critical, as it involves monitoring for signs of infection or complications. Reflection on these points is essential for improving surgical techniques and patient safety in future procedures.
Benefits and Risks of Humeral Interlocking Nail Surgery
Humeral interlocking nail surgery is becoming more common in orthopedic treatment. This technique offers several advantages. It is minimally invasive, which means less pain and quicker recovery. Studies show that patients typically regain functional use of their arms within weeks. Additionally, the procedure enhances bone stability, leading to lower fracture rates in some cases. According to a recent review, about 85% of patients experience satisfactory outcomes post-surgery.
However, despite these benefits, there are risks involved. Infection is a concern, occurring in up to 5% of surgeries. Complications may arise, such as nerve damage or nonunion of bones. Some patients report lingering discomfort or reduced range of motion, affecting daily activities. The psychological impact of surgery should not be overlooked. Patients may face anxiety regarding their recovery and potential complications, influencing their overall experience. Engaging in thorough discussions with medical professionals is crucial for setting realistic expectations.
Postoperative Care and Recovery for Humeral Interlocking Nail
Postoperative care following the insertion of a humeral interlocking nail is crucial for successful recovery. Research indicates that proper care can significantly impact the healing process. Patients typically need to maintain a restricted range of motion for several weeks. This limitation helps prevent complications like malunion. Active physical therapy is often recommended, but it should be approached with caution.
Pain management is a significant aspect of postoperative care. Many patients experience discomfort during the initial weeks. This discomfort can hinder their motivation for rehabilitation. Adequate pain relief techniques, including medication and alternative therapies, should be discussed. Additionally, a follow-up with the orthopedic surgeon is essential. Regular check-ups help ensure that the bone is healing correctly.
The recovery process can vary widely among patients. Some may regain full motion within three to six months, while others struggle for longer. Factors such as age, overall health, and compliance with rehabilitation play a role. It is vital to recognize setbacks, such as stiffness or prolonged pain, and address them with medical advice. Complications are possible, including infection at the nail site or blood clots, which emphasize the need for attentive postoperative monitoring.